The most common type of tongue malignancy is squamous cell carcinoma (SCC) which constitutes about 36.5% of all oral malignancies.1 It usually presents as painless swelling which is often ignored by the patient until late when it is symptomatic because of demonstrable growth in the oral cavity.2 Airway management in carcinoma posterior one third of tongue is always a concern to the anaesthesiologist due to possibility of trauma, bleeding, dislodgement of fractured tissue, chances of aspiration, difficulty in mask ventilation following induction of anaesthesia and compromised airway consequent to difficulty during laryngoscopy and intubation.3,4
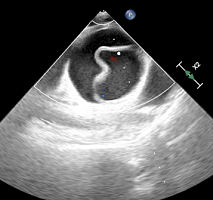
A 32-years-old, ASA grade I, female patient, regular tobacco chewer, presented with recurrent and gradually progressive intraoral polypoidal growth on right side of base of tongue. She was posted for excisional biopsy under general anaesthesia. Airway examination revealed adequate mouth opening with Mallampati grade II. The growth was obliterating the tonsillar fauces and pillars on right side but uvula and soft palate were clearly visible on phonation (Figure 1).
Figure 1. Showing Polypoidal Growth in Oral Cavity

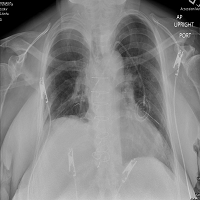
Findings of swelling were confirmed by magnetic resonance imaging (MRI) and computed tomography (CT) scan neck which showed polypoidal exophytic lesion at the base of posterior part of tongue in pre epiglottic space measuring 33x23x35 mm with separation of epiglottis from the growth involving right vallecula (Figure 2).
Figure 2. Showing CT Scan Neck Showing Polypoidal Exophytic Lesion at the Base of Posterior Part of Tongue

Anticipating difficult intubation, written informed consent was obtained for emergency tracheostomy and patient was shifted to the operation theatre and connected to a standard multipara monitors. Awake fibreoptic intubation was not performed initially because of unavailability of it in our institute at that time.
So instead we opted for video laryngoscope which was at hand for intubation under direct visualization.
After premedication and preoxygenation for 3 minutes, she was induced with intravenous (IV) fentanyl 2 mcg.kg-1 and IV Propofol 2 mg.kg-1 and IV suxamethonium 1.5 mg.kg-1 was administered after confirming adequacy of ventilation by bag mask ventilation. A nasal cuffed endotracheal tube (ETT) size 7.0 mm was passed through left nostril upto oropharynx and a video laryngoscope (King VisionTM) was introduced orally. Profuse bleeding started from the polypoidal mass which obscured the laryngoscopic view and hence video laryngoscopy was abandoned. Patient was immediately repositioned with a right lateral tilt and after appropriate suctioning, anaesthesia was deepened with Sevoflurane in oxygen on spontaneous respiration. Reintroduction of a conventional laryngoscope with McCoy blade and external laryngeal manipulation, helped in visualization of vocal cords and the trachea was intubated with cuffed oral ETT 6.5 mm after manipulation. Anaesthesia was maintained with Sevoflurane in oxygen and atracurium. After excision of polypoidal mass, residual neuromuscular blockade was reversed and trachea was extubated after patient was awake.
Difficult airway is the most common cause of morbidity and mortality during surgery of oral cavity malignancies. Flexible fibreoptic bronchoscopy with awake intubation is the gold standard in such anticipated difficult intubations, however friable growths may lead to profuse bleeding and difficulty in visualizing the larynx and subsequent intubation.4,5
Tracheal intubation in lateral position is difficult more so in right lateral as compared to left lateral position. Deterioration of the laryngeal view due to limited space between the laryngoscope handle and the table top in right lateral position contributes to difficult intubation with the conventional laryngoscope when the tracheal tube is inserted from the right corner of the mouth. In this case laryngoscopy with McCoy blade and intubation in right lateral instead of left lateral position was preferred as the bleeding mass was encroaching on right oropharynx.6 Secondly, laryngeal view is more hampered with the King VisionTM video laryngoscope as per our personal experience since introduction of the blade of video laryngoscope is more difficult in lateral position and the camera view is further compromised by fogging or pharyngeal blood. The width and angulation of the blade occupies more oropharyngeal space further reducing the laryngeal view. Though, the video laryngoscope with C-Mac blade has higher success rate of intubation in lateral position it is not available in our institute.7
So if advanced intubating aids are not available in case of anticipated difficult airway, we should manage such situations with airway equipments with which we are more familiar. Maintaining oxygenation throughout the procedure should always be ensured.
CONSENT
A written informed consent was obtained from the patient.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.