INTRODUCTION
Maintenance of the airway and adequate ventilation prior to endotracheal intubation is essential for the anesthetized patient. However, this may be compromised in patients with obesity or obstructive sleep apnea (OSA) due to partial or complete pharyngeal obstruction.1,2,3 In patients with facial trauma, craniomaxillofacial anomalies, or presence of external hardware, it may not be possible to achieve an adequate mask seal or perform bagmask-ventilation with a conventional facemask.4,5 For these patients and others with confirmed or suspected difficult airways, management alternatives including nasal ventilation may be more appropriate.3,6,7
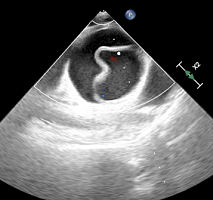
The SuperNO2 VA™ (Vyaire Medical, Mettawa, IL, USA) device is a nasal mask developed to provide nasal positive pressure ventilation in spontaneously breathing and apneic patients during anesthesia and endotracheal intubation (Figure 1). In a pilot study designed to evaluate the clinical performance of the SuperNO2 VA™ in paralyzed patients under general anesthesia, nasal mask ventilation was successfully implemented in 97% of patients with nasal oxygenation continued during laryngoscopy and orotracheal intubation, with no adverse events.6
Figure 1. Graphic Image of the SuperNO2VA™ Device.8

Much the same way nasal continuous positive airway pressure (CPAP) complements full facemask CPAP, nasal ventilation in apneic patients provides an alternative route to conventional techniques, improving the airway provider’s armamentarium. Additionally, mask seal is simpler to achieve with a nasal mask, using a smaller surface area and simply applying pressure to the mask into the face, whereas downward pressure of a full facemask may displace the mandible and soft tissues posterior into the upper airway.
Herein, we report an unusual case of a male patient with extruding mandibular hardware and facial fistula who presented for urgent surgery. Whereas a conventional facemask was not possible due to obstruction from the hardware, we document the use of the SuperNO2 VA™ device to provide pre-oxygenation and nasal ventilation during the induction of general anesthesia and endotracheal intubation. Written informed consent was provided for publication and photographs of this case.
CASE PRESENTATION
A 35-year-old male, American Society of Anesthesiologists (ASA) physical status III and weighing 70 kg (normal body mass index (BMI)), was scheduled for urgent removal of mandibular hardware, closure of left facial fistula, and multiple tooth extractions. The patient’s history was significant for poorly controlled seizure disorder, continued multiple substance abuse (alcohol and tobacco), recent pleural effusion of unknown etiology, and major depression. Notably, approximately six years prior to the current presentation, the patient sustained a self-inflicted gunshot wound to the left mandibular region. Treatment required a temporary tracheostomy and extensive facial reconstructive surgery, including the placement of mandibular hardware to replace lost structural tissue. After reconstruction, the patient was lost to follow-up. In the intervening years, numerous complications resulted from a combination of poor self-care and lack of medical care, including numerous infections, hardware erosion through the skin, several dental caries, and chronic pain. Consent for use of photography was obtained from the patient on the day of surgery.
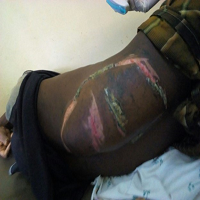
The pre-operative exam revealed a thin, adult male, appropriately nulla per os (NPO) without recent nausea, vomiting, recent upper respiratory infections, or obstructive respiratory symptoms or respiratory distress. He was visibly anxious and uncomfortable. The exam was remarkable for a nearly complete lack of mandibular structure and a large amount of hardware eroded through the skin where his mandible once existed (Figure 2). Mallampati evaluation to predict ease of endotracheal intubation could not be completed due to the patient’s oral pain.
Figure 2. Mandibular Hardware Seen Protruding through an Eroded Defect in the Face. The Exit Point Creates an Obvious Difficulty for Creating a Mask Seal with a Traditional Facemask

Anesthetic concerns focused on the potential for difficult intubation and ventilation, secondary to the lack of bony jaw structure and protruding hardware, which would interfere with mask seal and laryngoscopy. After consultation with the surgical team, both oral and nasal ventilation were deemed acceptable. All intubation possibilities, including awake fiberoptic intubation, were considered and thoroughly explained to the patient. The decision was made to pre-oxygenate with the SuperNO2 VA™ nasal mask, followed by gradual sedation and confirmation of successful mask ventilation prior to induction of general anesthesia and orotracheal intubation using a video-laryngoscope. Flexible endoscopic laryngoscopy was immediately available if video laryngoscopy failed. Emerging the patient and attempting awake fiberoptic intubation was planned if ventilation or laryngoscopy wa unsatisfactory or not possible.
The patient was given low-dose benzodiazepine, taken to the operating room and pre-oxygenated for five minutes using the SuperNO2 VA™ nasal mask. A titration of 50 mcg fentanyl, 100 mg lidocaine, and 120 mg propofol was given before the patient became apneic. To achieve adequate seal with the SuperNO2 VA™ and perform bag mask ventilation, the anesthesiologist placed his left-hand palm on the nasal mask and used digits 2-5 to provide head-tilt and deliver sub-mental pressure, driving the tongue against the hard palate to occlude the oral cavity (Figure 3). Bagmask-ventilatory support was successful and complete ventilation take-over was achieved following administration of additional propofol and fentanyl. Paralytic medications were not given. The case proceeded uneventfully, and the patient met extubation criteria at the end of surgery. The patient’s trachea was successfully extubated and he maintained appropriate respiratory parameters in the Post Anesthesia Care Unit with supplemental oxygen. He recovered without events and was discharged to the general wards without complication.
Figure 3. Sub-Mental Pressure Technique. Mask Seal is Created Using Downward Pressure Applied to the SuperNOVA Device. Using Two or More Digits, Firm Pressure is Applied to the Soft Tissue of the Sub-mental Space Driving the Tongue Cephalad Against the Hard Palate, Occluding the Oral Cavity from Within

DISCUSSION
Maintenance of the airway and ensuring adequate ventilation are among the chief concerns in the surgical arena during the induction of anesthesia. Patients presenting for surgery under general anesthesia with endotracheal intubation endure a brief period of apnea upon induction and when the facemask providing ventilation is removed for access to the oral cavity for orotracheal intubation. Most patients tolerate this brief apneic period well and pre-oxygenation is often used to extend this period. However, it is not always possible to predict a difficult airway or other issues that may arise, placing patients at risk for desaturation. Patients who are obese, pregnant, suffer from chronic OSA, and/or pediatric cases may be at higher risk for this complication.1,2,3 Similarly, for patients with craniomaxillofacial dysmorphology or trauma, anesthesiologists may be unable to achieve an adequate seal with a conventional facemask,4,9,10 placing the patient at greater risk for desaturation due to inadequate ability to bag-mask-ventilate and intubate.
In the current case, a detailed pre-operative airway exam including the Mallampati assessment could not be performed, due to the patient’s reported oral pain, preventing an accurate assessment of the risk for difficult intubation. Additionally, the exposed mandibular hardware precluded the use of a conventional facemask to provide adequate ventilation. Therefore, to meet the ventilation needs of the patient before and during intubation, nasal ventilation was performed. Alternatively, intubation via flexible endoscopy while awake or under sedation should be considered an option for these situations. Given the quantities of sedative medication necessary to overcome the patient’s pain and discomfort, along with the experience and expertise the team has using nasal ventilation in apneic patients, flexible endoscopy was kept immediately available while a controlled induction with gradual nasal ventilation takeover was preferred.
Nasal ventilation has been observed to reduce airway obstruction compared to oral-nasal ventilation in patients undergoing general anesthesia.11 More recently, Ghebremichael and colleagues evaluated the use of the SuperNO2 VA™ during anesthesia induction and throughout laryngoscopy. In all but one patient, anesthesiologists were able to use the SuperNO2 VA™ to provide adequate ventilation during induction and laryngoscopy.6 The SuperNO2 VA™ provides non-invasive, continuous ventilation via the nasal route, via the buildup of positive pressure in the nasopharynx, anteriorly displacing the soft palate and tongue from posterior pharyngeal wall, reducing airway obstruction. Use of the SuperNO2 VA™ for pre-oxygenation and during induction may reduce the risk for oxygen desaturation in patients with obesity or OSA, as well as patients with other comorbidities that are associated with difficult intubation.6
CONCLUSION
A conventional facemask could not be used on this patient for pre-oxygenation, mask ventilation, or maintenance of oxygenation during the apneic period due to extruding mandibular hardware and facial fistula, which precluded the creation of an adequate seal. A nasal-interface device, the SuperNO2 VA™, was successfully used for preoxygenation and to provide ventilation during induction of general anesthesia without event. The SuperNO2 VA™ device may be an appropriate choice to protect against respiratory insufficiency in the peri-operative period for patients with pan-facial trauma, craniomaxillofacial anomalies, or presence of mandibular hardware when conventional facemask is not recommended.
ACKNOWLEDGMENTS
Support for this publication was provided by Vyaire medical. Writing assistance, funded by Vyaire Medical, was provided by Jennifer Malinowski, PhD of Write InSciTe, LLC and Linda A. Goldstein, PhD, CMPP of The Write Source MSC, LLC. AUTHORS’ CONTRIBUTIONS M.M. and G.K. have contributed to the conception and design of the report, drafting and revision of this manuscript, and have given final approval for submission.
CONSENT
The authors have received written informed consent from the patient.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.